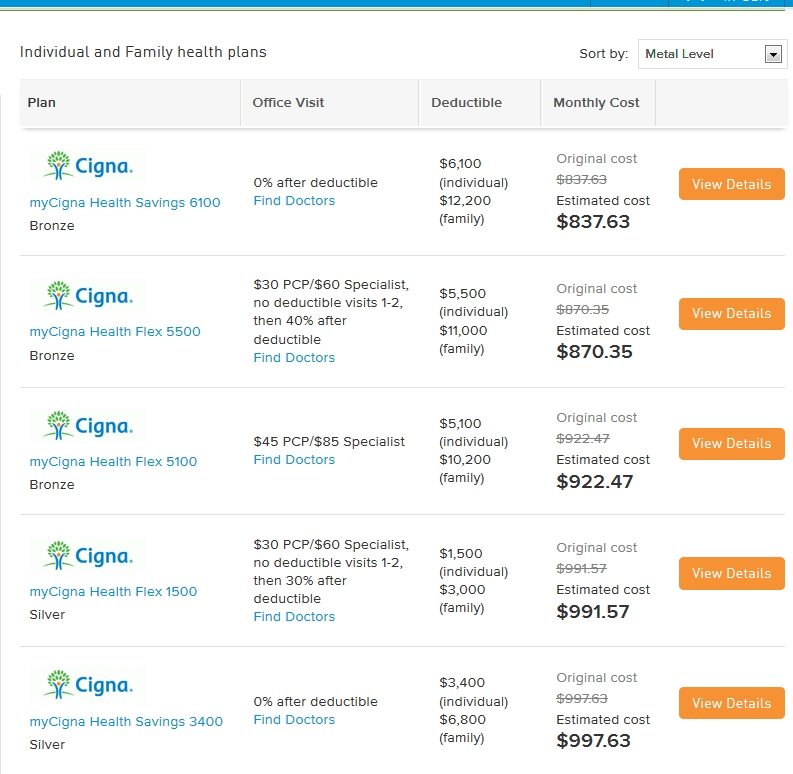 
Simply put, it has a low chance of appeal after you’ve received the denial, thus you lose money. I just need a hardcopy of their billing policies for PAs, it shouldn't be this hard to find, should it Any help is appreciated. I understand that Cigna does not credential PAs, and when I ask for policies, I'm directed to their website. cigna timely filing limit 2021grace and frankie eating. Submitting a claim past an insurance's timely filing limit will come back to you as Claim Adjustment Reason Code (CARC) 29 and state, “The time limit for filing has expired.”ĬARC 29 has a high chance of prevention but a low overturn rate. 1 I have looked and can not find Cigna's policy for billing physician assistants. If you have a question concerning a previous Cigna Member, claim. On the flipside, if your team isn't familiar with the limits for the insurances the majority of your patients use, you're losing revenue. Knowing the deadlines of payers that attribute to most of your revenue before your patients visit your office will help your team anticipate and submit your claims faster. Why not use it as a guide to help identify the most important timely filing limits your team should be aware of? It's helpful in breaking down what percentage of revenue comes from common insurances. When speaking to our clients, most of them know their payer mix.Ī payer mix is a listing of the different healthcare insurances your patients use. But which are they actually using? Of course, I'm referring to what's known within the industry as a "payer mix." There are hundreds of thousands of insurance options your patients can choose from. Some of those responsibilities include patient care, coding, and keeping track of healthcare requirements.Įnsuring your team is submitting patient claims on time is another important responsibility you need to know. With a small amount of extra effort, you can lower your timely filing denial rate even more.Ĭhances are, you and your staff already have a ton of work to complete on a daily basis. As a simple example for reference, 0.01% of $3,000,000 is $30,000.įurthermore, that percentage is only true if you have all of those payers and submit an equal amount of claims to each. If the deadline isn’t 180 or 365 days then there’s a 56% chance that the limit is 90 daysīy submitting your claims within 90 days the chances that you receive a claim denial related to timely filing is 0.01%.Ī 0.01% chance stacks the odds in your favor, although that percentage can still have a significant negative effect on your bottom line if you aren't vigilant. If the deadline isn’t 180 days then there is a 46% chance that their limit is 365 days There is a 34% chance that an insurance company has a deadline of 180 days The two most popular timeframes are 180 days and 360 days In case, you’re looking for some additional information, feel free to contact us or comment below.From the bar graph and statistical data above we can conclude that…  
In this article, I have mentioned everything you need to know about timely filing limit along with the timely filing limit of all major insurances in United States. Also ask your accounts receivable team to follow up on claims within 15 days of claim submission. If insurance company allows electronic submission then submit claims electronically and keep an eye on rejections. To avoid timely filing limit denial, submit claims within the timely filing limit of insurance company. How to avoid from claim timely filing limit exhausted? What if claim isn’t sent within the timely filing limit?įailing to submit a claim within the timely filing limit may result in the claim being denied with a denial code CO 29, so it is important to be aware of the deadline and submit the claim promptly. A claim with a date of service after Mawill be held to standard plan timely filing provisions. Unitedhealthcare Non Participating Providers A claim with a date of service after Mabut before March 1, 2021, would have the full timely filing period to submit the claim starting on March 2, 2021. Keystone First Resubmissions & Corrected Claimsġ80 Calender days from Primary EOB processing dateġ2 months from original claim determination Amerigroup for Non Participating Providers
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
